Internationally known for global humanitarian work, Doctors Without Borders has for decades provided first responder health care to thousands of people around the world with the greatest immediate need. And while it might seem standard to hear about MSF — the nonprofit's French abbreviation, Medecins Sans Frontieres — distributing aid in a foreign country, the novel coronavirus has brought the organization closer to home: Southeast Michigan's nursing homes, to be exact.
Identifying a Need
Heather Pagano is MSF's emergency coordinator for Michigan. She said that while the U.S. is a very "high-resource" setting overall, the rate of infection in this part of the state was significant enough to warrant deployment — particularly because the rate of COVID-19 infection among older adults is especially high. When MSF finds a nursing home in need of its services, the process begins with a site assessment.
"We start by going into the nursing home and then we do a quick assessment that takes about an hour or two hours — often with the director of nursing or from the administrator or the environmental staff, and we just see where [there could be vectors for infection]. Because often, just an external pair of eyes [can be helpful]," she said. "When you're in it all day every day, maybe you don't see everything."
Pagano said that even a single in-person walkthrough of a facility is a great way to catch unconscious and accidental actions that could be helping to spread COVID-19 — even something a seemingly benign as the continuous readjustment or touching of a mask. When asked about the most common "weak spots" for infection, Pagano said it's often a lack of education for the cleaning or environmental staff. That's a trend she's seen in health care organizations around the world.

A member of the MSF team responding to the COVID-19 outbreak in New York City assembles water jugs for hand-washing stations. MSF has donated over 80 hand-washing stations to essential places like soup kitchens and supportive housing facilities in New York City. United States 2020 © Michelle Mays/MSF
"So often [training] focuses on nurses, but actually, it's cleaning staff or nurse aids who have a lot of interaction and close contact with residents that also need training, but they're maybe only an afterthought," Pagano said. "Or if you have limited resources you direct it toward the medical staff, not the nonmedical staff. But the nonmedical staff also need to understand the virus in order to protect themselves. … If you want to affect behavior change in people, you can't just tell them what to do, you have to explain to them why they should do it."
Not Handing Out Tickets
Pagano added that the intention of MSF doing walkthroughs of nursing homes is not to emphasize what an organization is doing wrong.
"We're not here to give you citations. We're not here to tell you all the things that are wrong to give you fines. We're here to give you an extra bit of support," she said. "For me, that's really at the core of humanitarianism, which is what we do all over the world, but I think just being with these people and letting them know that they're not alone [is valuable]."
After the initial walkthrough is finished, a tailored experience is created for each chosen facility. That experience can mean anything from providing mental health workshops for employees dealing with added work stressors due to COVID-19, on-site support when necessary and COVID-19-specific staff trainings. So far, of Southeast Michigan's 26 nursing facilities, MSF has done "11 site assessments, 11 training and four [personnell] embeds and four mental health sessions."
One of five projects across the U.S., Southeast Michigan's is the only one that is targeting nursing homes. In addition to that, Pagano said that MSF is hoping to help curb COVID-19 cases that have disproportionately affected people of color.
"According to the data that was just released last week from the state health department, African Americans make up 14 percent of the population but they're about 1/3 of positive cases and 40 percent of the deaths in Michigan. So, it is affecting communities of color disproportionately in communities of color across the U.S. That is the case here in Michigan for a variety of different reasons," Pagano said. "COVID has taken a heavier toll in the urban setting, and Detroit is predominantly African American. And then, of course, all of the racial disparities and access to health care, comorbidities and all of these underlying factors have contributed to this disproportional impact. It's another reason for [our] intervention in Michigan. We always strive to go where we can be of help and where there are disparities and issues in access to health care."
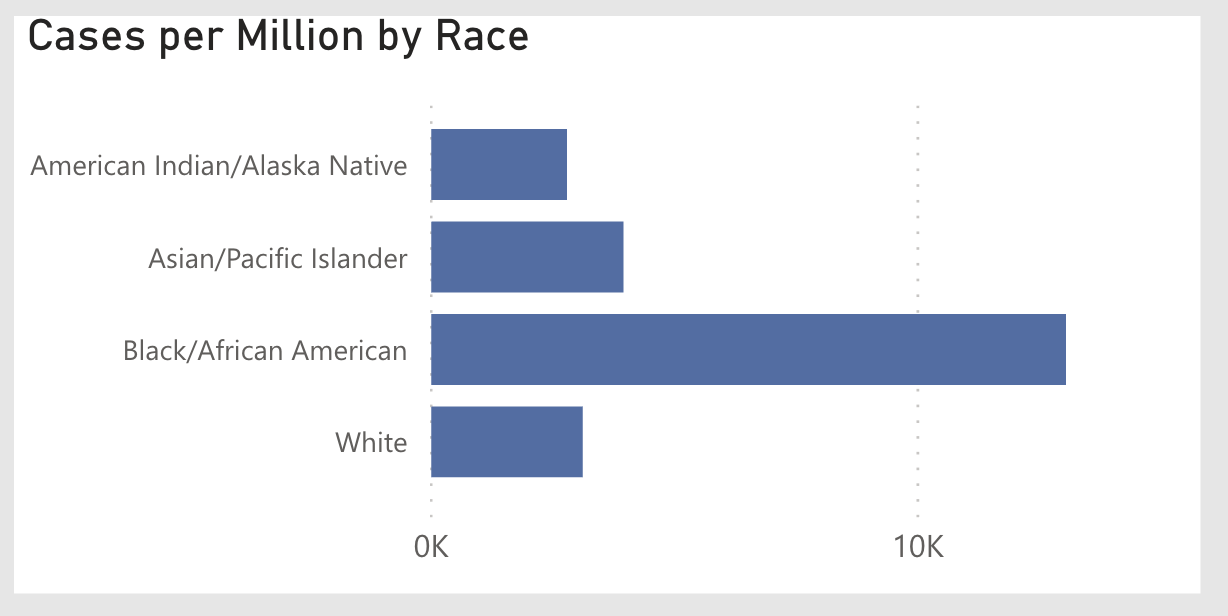
Of Michigan's confirmed 70,000-plus cases, the vast majority of those affected have been people of color. Find Michigan's latest COVID-19 infection data online at gaybe.am/wT
When asked how long MSF will be in the area, Pagano said that it depends on the organizations being helped, but that MSF will be aiding organizations as long as they are in need of guidance. Some, she said, simply are in need of extra staff — and have been for long before the pandemic — which Pagano's team cannot provide.
"Not everybody needs it and not everybody wants it, and that's the idea as well. If they say, ‚ÄòWhat we need is more staff, not trainings,' then that's fair enough because I don't have staff that I can embed with you right now," she said. "Other places say that we could really use the help. It's a voluntary approach. … We could go to some facilities as many as four or five times if they have a variety of different types of staff, and it also depends on their schedule, of course."
But for those nursing homes that will benefit from MSF's aid, it can be a welcome reprieve from a packed patient schedule — and a great way to prepare to reopen when Michigan's coronavirus restrictions loosen.
"It's important that we try to help these facilities in this delicate moment before that begins," Pagano said. "And the fact that people can't see their relatives, that part needs to be done as safely as possible, but also as quickly as possible in some cases, because people really suffer without being able to see their families. It's important that we try to help these facilities in this delicate moment before that begins."
To learn more about MSF's impact in Michigan click here.










